A Day In The Life Of A Transplant Nurse Practitioner
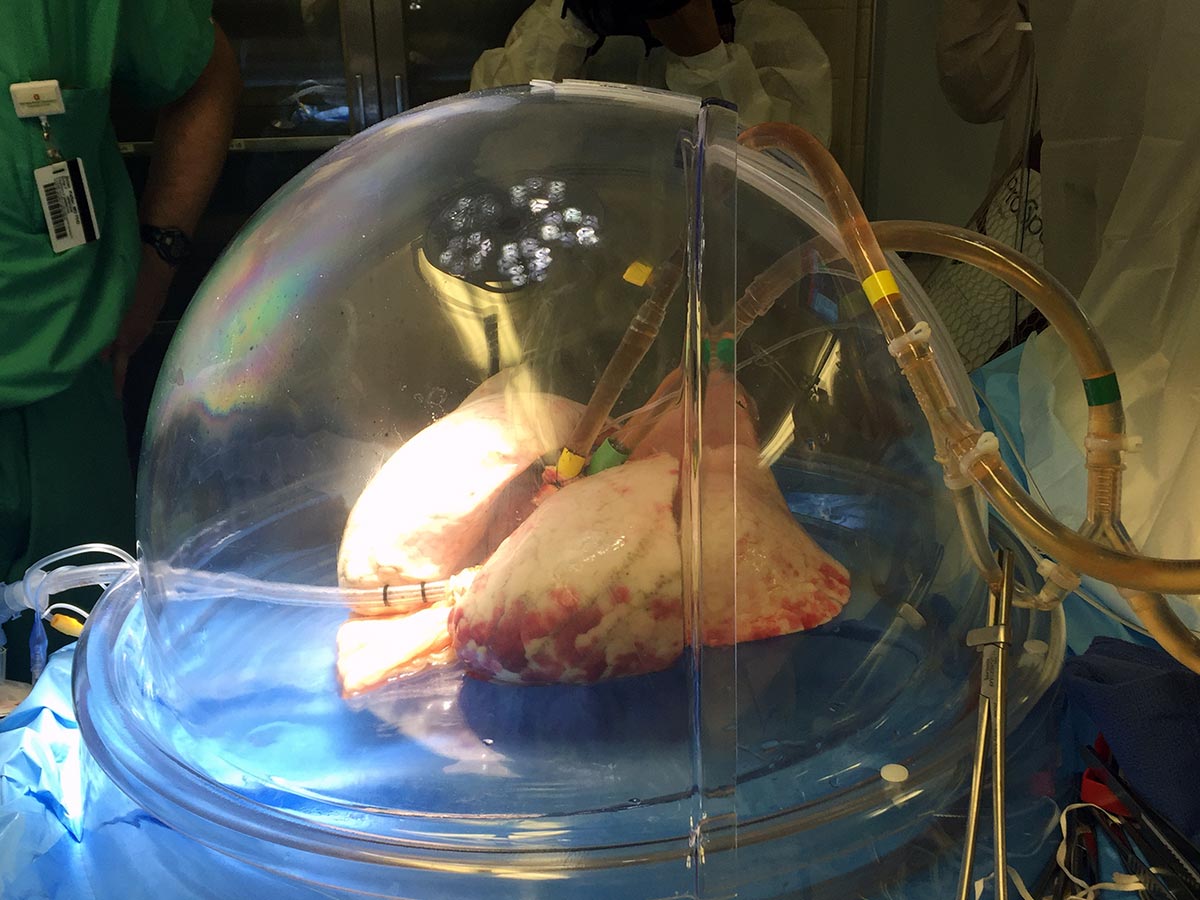
Nurse practitioners are well positioned to provide consistent, quality care to those with chronic illnesses, and lung transplant medicine is no exception.
At Michigan Medicine in Ann Arbor, I have the privilege of caring for our pre- and post-transplant patients in the inpatient setting. Our group of 14 advanced practice providers have an expertise in the care of cystic fibrosis, ILD, COPD, lung transplantation, as well as the chronic use of invasive and non-invasive ventilatory support. As an NP, I develop relationships with patients and their families across the transplant continuum, and provide the specialized care these patients require. Pursuing an advanced practice career in lung transplant was fitting for me, as I have previous nursing experience in bone marrow transplant, pulmonology, and medicinal intensive care.
My typical day (though anyone in health care knows there is no such thing as typical!) begins at 0700am when our night shift providers hand off to the oncoming day shift, and then each of us individually prepares for rounds.
I review a patient’s history, recent events, and objective data. My assignment, usually about 5-7 patients, may include an ILD patient on high amounts of oxygen awaiting transplant, a recent post-transplant patient, and a transplant patient with an opportunistic infection. I pre-round on my patients to collect subjective data and examine them. I formulate a plan for the day and present this to our multidisciplinary team for discussion on rounds. Our rounding team includes a transplant pulmonologist, a transplant pharmacist, an outpatient nurse coordinator, and the bedside nurse when possible.
My role is to then carry out this plan over the course of the afternoon. Our APPs function with a high level of autonomy; our attendings are available to us throughout the day as needed. I manage antibiotics and immunosuppression. I coordinate scheduling of bronchoscopies with our procedural unit. I spend much time collaborating with consulting services, such as Transplant Nephrology and Infectious Disease. I also spend time in the afternoon admitting patients from outside hospitals, home, or our emergency department. I collaborate with our thoracic surgery team (APPs, residents, and fellows) in the transfer of post-surgical patients to our transplant medicine service. The team effort that goes into caring for this complex population is simultaneously challenging and rewarding.
Outside of my direct work with patients, I recently joined our lung transplant quality improvement committee.
I also had the opportunity to attend the Chest conference last year, which offered great learning and networking opportunities in the transplant community. At Michigan, an interdisciplinary group of my colleagues is working on standardizing our process for referring and evaluating cystic fibrosis patients for transplant. I am confident such efforts are being driven by pulmonary APPs in transplant centers across the globe. My hope is to develop partnerships, through organizations such as APAPP, in order to improve the care of those with end stage lung disease.

Leave a comment